Ukraine reports 5,276 new COVID-19 cases
Ukraine reports 5,276 new COVID-19 cases
 Zelensky: Every third Ukrainian considers road construction one of greatest achievements of 2021
Zelensky: Every third Ukrainian considers road construction one of greatest achievements of 2021
 Ukraine ready to implement Minsk agreements, but Russia's desire needed - Yermak
Ukraine ready to implement Minsk agreements, but Russia's desire needed - Yermak
 Michel: EU unanimously agree to roll over economic sanctions against Russia
Michel: EU unanimously agree to roll over economic sanctions against Russia
 Actions by Ukraine's partners will help prevent worst-case scenario - Zelensky
Actions by Ukraine's partners will help prevent worst-case scenario - Zelensky
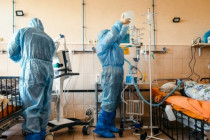 COVID-19 in Ukraine: Health officials confirm 8,899 daily cases as of Dec 17
COVID-19 in Ukraine: Health officials confirm 8,899 daily cases as of Dec 17
 Macron tells Zelensky he declared support for Ukraine in call with Putin
Macron tells Zelensky he declared support for Ukraine in call with Putin
 Zelensky, Scholz discuss gas transit through Ukraine after 2024
Zelensky, Scholz discuss gas transit through Ukraine after 2024
 Ukraine ready for any format of talks with Russia - Zelensky
Ukraine ready for any format of talks with Russia - Zelensky
 Ukraine’s only journalist in Russia facing extremism charges - lawyer
Ukraine’s only journalist in Russia facing extremism charges - lawyer
 PM Shmyhal: First two applications for investment projects worth $96 million filed
PM Shmyhal: First two applications for investment projects worth $96 million filed
 Zelensky, PM of Italy discuss security situation around Ukraine
Zelensky, PM of Italy discuss security situation around Ukraine
 President signs off State Budget 2022
President signs off State Budget 2022
 London considering all options for responding to Russia's aggression against Ukraine
London considering all options for responding to Russia's aggression against Ukraine
 Putin, Biden to hold another round of talks
Putin, Biden to hold another round of talks
 Some 260,000 Ukrainians “victims of human trafficking” over 30 years - prosecutor general
Some 260,000 Ukrainians “victims of human trafficking” over 30 years - prosecutor general
 Ukraine plans to create center to protect energy infrastructure from cyber attacks
Ukraine plans to create center to protect energy infrastructure from cyber attacks
 No clear idea so far when Normandy Four top diplomats set to meet - German Ambassador
No clear idea so far when Normandy Four top diplomats set to meet - German Ambassador
 Ukraine receives EUR 600M in macro-financial assistance from EU
Ukraine receives EUR 600M in macro-financial assistance from EU
 Zelensky holds phone conversation with PM of Israel
Zelensky holds phone conversation with PM of Israel
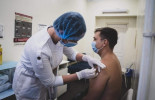
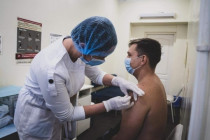 Ukraine sets new daily COVID vaccination record
Ukraine sets new daily COVID vaccination record
 MFA: European Union has not yet removed Ukraine from list of safe countries
MFA: European Union has not yet removed Ukraine from list of safe countries
 Kyiv records 1,023 new COVID-19 cases, 29 deaths
Kyiv records 1,023 new COVID-19 cases, 29 deaths
 G7 ambassadors welcome adoption of law on NABU status
G7 ambassadors welcome adoption of law on NABU status
 Ukraine can increase Covid vaccination rates to 1.5M a week – Liashko
Ukraine can increase Covid vaccination rates to 1.5M a week – Liashko
On a doorstep in the suburbs of north London, three-year-old Ayse picked up a tissue to wipe away her grandmother’s tears - tears for one more victim of the virus.
The little girl was waiting for her mum, Sonya Kaygan. Her grandmother hadn’t broken the news that Kaygan, 26, who worked at a nearby care home, was dead, one of over 100 frontline health workers killed by the coronavirus in Great Britain.
The grandmother, also called Ayse, spoke through sobs. “Why? Why?” she repeated. Why couldn’t she visit the hospital to say her goodbyes? Why did so many die in her daughter’s workplace? At least 25 residents since the start of March, of whom at least 17 were linked to the coronavirus. It was one of the highest death tolls disclosed so far in a care home in England. And why did Kaygan and her colleagues resort to buying face masks on Amazon a month ago, protection that arrived only after she was in hospital?
A Reuters investigation into Kaygan’s case, the care home where she worked, and the wider community in which she lived provides an intimate view of the frontline of Britain’s war on the coronavirus. It exposes, too, a dangerous lag between promises made by Prime Minister Boris Johnson’s government and the reality on the ground.
Even as the government was promising to protect the elderly and vulnerable from the deadly virus, local councils say they didn’t have the tools to carry out the plan, and were often given just hours to implement new government instructions.
Policies designed to prevent hospitals from being overwhelmed pushed a greater burden onto care homes. With hospitals given priority by the government, care homes struggled to get access to tests and protective equipment. The elderly were also put at potentially greater risk by measures to admit only the sickest for hospital treatment and to clear out as many non-acute patients as possible from wards. These findings are based on documents from government agencies seen by Reuters, interviews with five leaders of local authorities and eight care home managers.
It is too early to reach final conclusions about the wisdom of these policies. Still, staff and managers of many care homes say they believe the British government made a crucial early mistake: It focused too much attention on protecting the country’s National Health Service at the expense of the most vulnerable in society, among them the estimated 400,000 mostly elderly or infirm people who live in care homes across Britain.
The government summed up that policy in the slogan “Protect the NHS.” The approach gave the country’s publicly-funded hospitals priority over its care homes. A UK government spokesman defended the strategy. “This is an unprecedented global pandemic and we have taken the right steps at the right time to combat it, guided by the best scientific advice.”
The effects of this approach have been felt desperately in Elizabeth Lodge, in Enfield, north London, where Kaygan worked.
The first coronavirus test of a resident of the Lodge only took place on April 29. That was 34 days after the first suspected case at the home, said Andrew Knight, chief executive of residential services at CareUK, a private company which operates the home. It was also 14 days after Matt Hancock, the UK health secretary, pledged tests would be available to “everyone who needs one” in a care home.
“The government’s response on testing has come way too late to have any meaningful effect on keeping the virus out of our homes,” said Knight, the CareUK executive, in a statement to Reuters.
So far, at least 32,300 people have died in Britain from the coronavirus, the highest toll in Europe, according to official UK data processed by 2 May. Out of those deaths, more than 5,890 were registered as occurring in care homes in England and Wales by April 24, the latest date available. These figures don’t include care home residents who were taken to hospital and died there.
Many care home providers believe the figures understate the number of deaths among care home residents because, in the absence of testing, not all are being captured. During the 10 weeks prior to the outbreak, including the height of the flu season, an average of 2,635 people died each week in care homes in England and Wales. By April 24, that weekly death toll had risen to 7,911. According to Reuters calculations, the pandemic has resulted in at least 12,700 excess deaths in care homes.
“I think the focus early on was very much on the acute sector,” or urgent hospital treatment, “and ensuring hospitals were able to respond in an effective way,” said Graeme Betts, acting chief executive of Birmingham City Council, which oversees the UK’s second-biggest city. “And I think early on care homes didn’t get the recognition that perhaps they should have.”
Helen Wildbore, director of the relatives and residents association, a national charity supporting families of people in residential care, said while it was right for the initial focus to be on protecting the NHS, “I think it has taken too long for the government to turn its attention” to vulnerable people outside hospital. “I think it’s fair to say that the sector has felt like an afterthought for quite a long time.”
Jeremy Hunt, a former Conservative Party health secretary and now chairman of the House of Commons health select committee, advocated banning visits to care homes by friends and family from early March, advice that wasn’t followed. Speaking to Reuters, he drew a parallel between the UK’s response to the coronavirus and the way it deals with peak winter demand for hospital services.
“What happens with any NHS winter crisis is the focus of attention immediately switches to the hospitals and dominates the system’s thinking,” he said. “Many people in the social care sector told me exactly the same thing happened with COVID-19.”
The government spokesman said protecting the elderly and most vulnerable members of society had always been a priority, “and we have been working day and night to battle coronavirus by delivering a strategy designed to protect our NHS and save lives.”